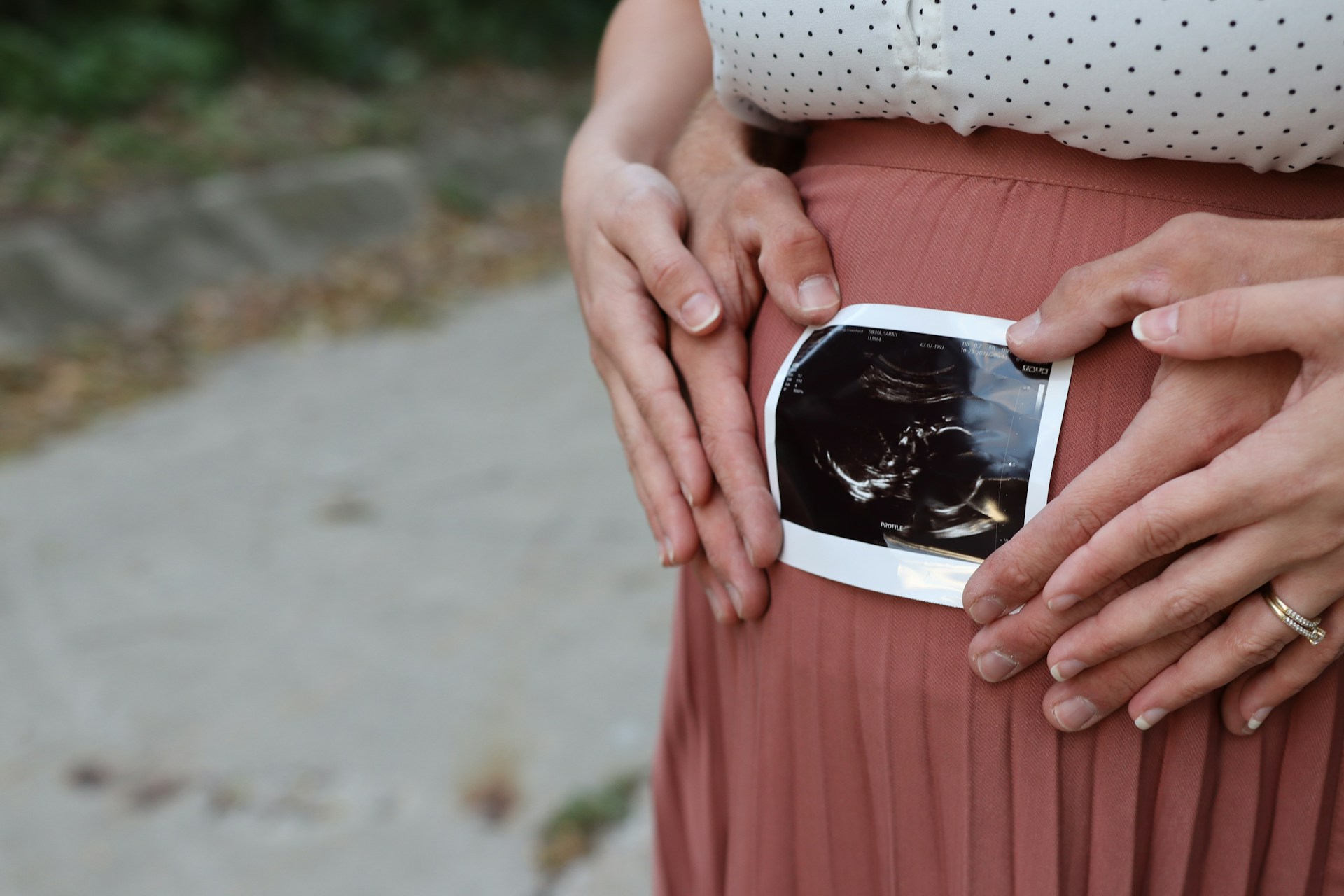
Expectant mothers face numerous physical and emotional shifts during pregnancy, requiring consistent and reliable medical attention.
Geographic barriers, busy schedules, and a shortage of specialists often prevent patients from receiving the attention they need. Telemedicine has emerged as a practical solution to these challenges, fundamentally changing how healthcare systems deliver maternal support.
By shifting appointments from physical waiting rooms to virtual platforms, clinicians can maintain a continuous connection with their patients. This evolution introduces digital pregnancy care to communities that previously lacked sufficient medical infrastructure.
It also provides immediate remote OB support for critical questions that arise between scheduled appointments. The integration of these virtual services represents the future of obstetrics, creating a safer and more accessible environment for mothers nationwide.
1. Expanding Access for Every Patient
Breaking Down Geographic Barriers
Mothers living in rural or underserved areas often travel hours to see an obstetrician. Telehealth eliminates this commute by facilitating virtual consultations. Patients simply log into a secure portal to discuss symptoms, review test results, and receive guidance from a qualified physician.
Key benefits of expanded virtual access include:
- Reduced travel time and associated costs
- Decreased exposure to communicable illnesses in waiting rooms
- Increased frequency of routine check-ins
2. Enhancing the Prenatal Experience
Consistent Monitoring from Home
Routine prenatal visits are vital for tracking the growth of the fetus and the health of the mother. Through virtual platforms, clinics can offer comprehensive digital pregnancy care that complements physical examinations.
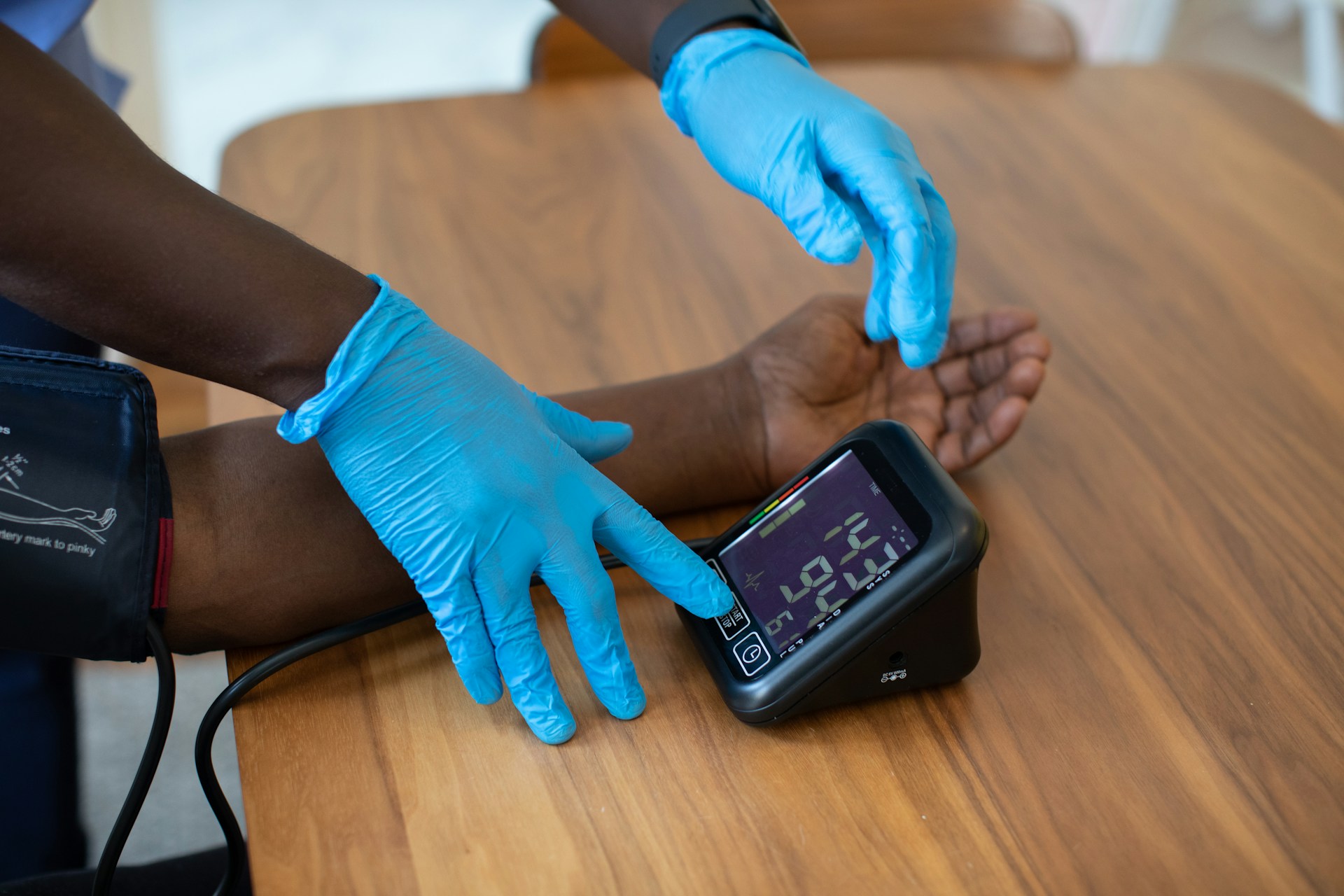
Patients use home medical devices, such as blood pressure cuffs and fetal dopplers, to transmit health data directly to their providers. This continuous stream of information allows doctors to detect potential complications early and adjust treatment plans accordingly.
3. Managing High-Risk Pregnancies Remotely
Keeping Families Close to Home
High-risk pregnancies require specialized maternal-fetal medicine (MFM) expertise. Telehealth connects these vulnerable patients with board-certified MFM specialists, 24/7/365. This immediate access to remote OB support reduces the need to transfer patients to distant specialist facilities.
Families can stay close to their support networks while receiving expert care. Real-time consults ensure that local providers have the specialized backing they need to manage complex cases safely.
4. The Role of Providers in the New Era
Seamless Clinical Collaboration
Telemedicine does not replace local physicians; it empowers them. General obstetricians and local hospital staff can collaborate with remote specialists to deliver comprehensive treatment plans.
This collaborative model is a defining feature of the future of obstetrics, allowing clinicians to practice with purpose and impact. By sharing data and insights through secure virtual networks, healthcare teams can coordinate responses to emergencies and improve overall maternal outcomes.
5. Navigating the Postpartum Period
Continuous Care After Delivery
The weeks following childbirth are often the most challenging, yet they traditionally receive the least clinical oversight. Telehealth platforms provide a vital lifeline during the postpartum period.
Mothers can connect with lactation consultants, mental health professionals, and obstetricians without leaving their homes.
This extension of digital pregnancy care ensures that issues like postpartum depression, infection, or breastfeeding difficulties are addressed promptly, safeguarding the health of both mother and baby.
6. Technology Shaping the Next Decade
Integrating Wearables and Artificial Intelligence
As technology advances, remote OB support will become even more sophisticated. Wearable health monitors that track maternal heart rate, sleep patterns, and physical activity are already providing clinicians with actionable data.
Furthermore, artificial intelligence can analyze this data to predict complications before they escalate. Embracing these innovations is crucial for healthcare systems that wish to lead the future of obstetrics and provide the highest standard of patient care.
A New Standard for Maternal Wellbeing
The integration of virtual health solutions into standard obstetric practice is making care safer, closer, and more accessible.
By equipping local hospitals with specialized virtual support and allowing mothers to receive expert consultations from home, the healthcare industry is closing critical gaps in maternal-fetal medicine.
If you are a healthcare provider or a hospital administrator looking to integrate these advanced solutions into your practice, learn more about how innovative partnerships are redefining maternal health.